Under the microscope: Newsday writer takes a sperm test

After sitting in the waiting room came the walk along the corridor to the changing room to put on scrubs – which I was later told feels like the "walk of shame" for most men. It certainly caused me some anxiety. It inspired the seemingly inevitable thought: "Could something be wrong with me?"
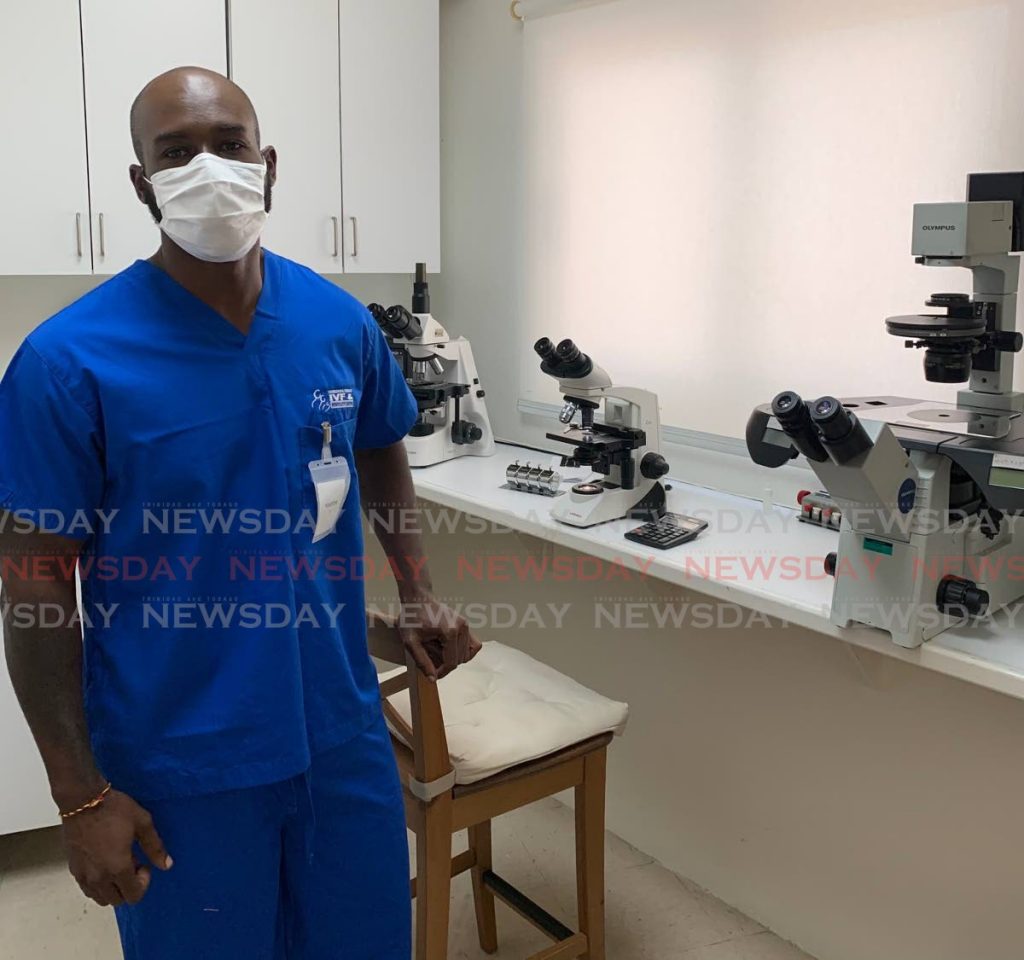
I was visiting the Trinidad and Tobago IVF and Fertility Centre in Maraval, where I got to sit with science director and embryologist Natalie Jess and fertility nurse, andrology technician, phlebotomy technician and patient support group co-ordinator Gabrielle Rodney.
And, being a man, I got a first-hand experience of sperm analysis.
Asked how I felt, I told Rodney, "I'm definitely trying to be mentally prepared for whatever story might unfold here."
Getting the sample, which I took for granted was the easiest part, is in fact, according to Rodney, sometimes another challenging part of the emotionally enormous process for many men.
She said even producing a sample can mean 30 minutes or as much as an hour of nerves. For most men, even a visit to the centre only happens after having experienced conception challenges for some time. Jess and Rodney said in most cases, men come in after having tried to conceive for a while, and a sperm test isn't the first check.
The reluctance to be tested, Rodney said, may have much to do with the culture of the region – and the idea that less-than-perfect sperm health may be linked to being "a real man."
Asked if the centre has a in-house psychotherapist to help men with the mental enormity of the process, Jess said arrangements are made for men to speak with therapists, especially if treatment such as IVF becomes an option.
Jess said the anxiety men experience is usually intensified by the wait. Unlike my experience of going for testing, men usually give their samples, then wait a number of days for their results.
Rodney said the amount of sperm and its physical features help determine sperm health.
She explained the three basic parts of sperm; the head, which houses the nucleus where genetic coding/DNA is held, is capped by the enzyme containing acrosome that dissolves the egg; the midpiece, with the mitochondria which produces energy; and finally, the tail, which works as a propeller.

Rodney said the health of sperm is also determined, in part, by the average number found in semen without defects to these physiological parts. It is normal for men to find defects in some sperm.
"When doing sperm analyses we check for the sperm count; count of the motility, which refers to its ability to swim; and check the shapes. The three tests tell if sperm is normal or if there might be an issue."
Also, she said, "The volume is really important. A low volume could mean there is a blockage, and very high volume could mean seminal glands are hyperactive. The normal volume is between 1.5 and five millilitres."
She added that the sample should not be clear.
One myth they dispelled was that sperm retention is good for sperm health. On the contrary, Jess said sperm produced and retained for five days or longer are more likely to have breakages in the double helix, while recently produced, fresh sperm will be of the best quality.
The sample was then placed in a counting chamber, which gives the number of sperm per millilitre and also information on the rate of movement. This is done by observing sperm under a microscope.
Jess walked in to see Rodney clicking away at the counter as sperm swam under the microscope. I was relieved to hear that was a good sign. Viewing the sperm under a microscope for the first time was surreal.

The second test involved testing the sample with anti-sperm antibodies, which tests sperm's resistance and ability to bind with eggs. It may also indicate possible causes of issues such as infections or injury.
The third test was to check morphology, which basically means checking for consistency in healthy sperm, where all the parts are intact, proportionate and functional. There are instances where some parts of the sperm are underdeveloped or absent. Rodney said, on average, if one in every four sperm from a sample of 200 is a healthy one, there is nothing to worry about.
Jess also explained there is also a test called a sperm defragmentation, where DNA (molecules carrying genetic information) is analysed for possible breakages in its double-helix structure, which generally contributes to infertility.
The analysis has shown its importance for finding the cause of fertility problems and addressing them, despite how traumatic it may be for men.
The above article is writer Marshelle Haseley's concluding look at male infertility in Trinidad and Tobago. See link to his report https://newsday.co.tt/2021/07/18/men-take-a-sperm-test-why-male-infertility-is-high-in-trinidad-and-tobago/


Comments
"Under the microscope: Newsday writer takes a sperm test"